Phalanx Fracture
What is a Phalanx Fracture?
A Phalanx fracture is a break or crack in one of the bones (or phalanges) of your fingers. Each finger has three phalanges — proximal, middle and distal. The thumb has two. These fractures are among the most common hand injuries. They can result from everyday accidents like crushing your finger in a car door, taking a hit during a contact sport, or losing your balance and falling.
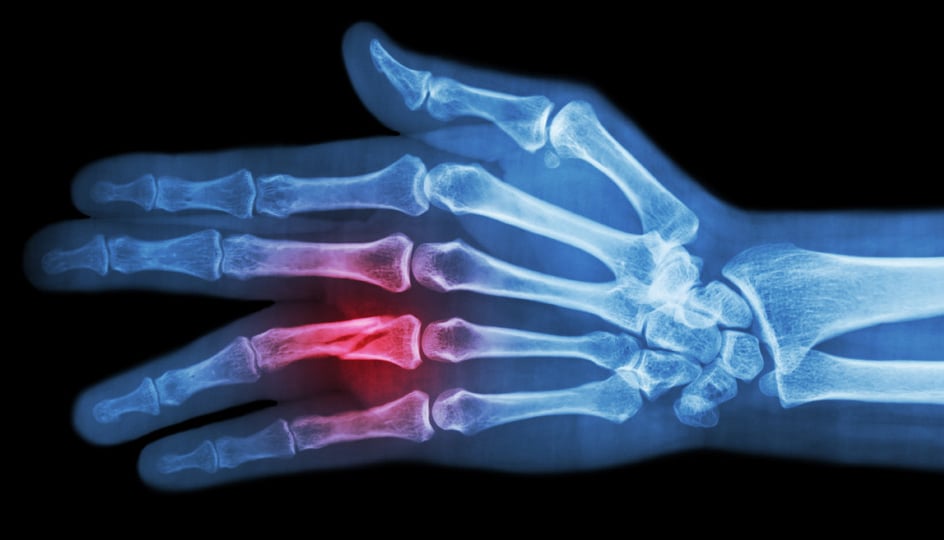 X-ray Showing a Phalanx Fracture
X-ray Showing a Phalanx Fracture
Symptoms
Symptoms of a phalanx fracture usually include one or more of the following:
- Finger pain and tenderness
- Finger swelling/stiffness
- Finger bruising
- Finger deformity (crooked fingers, end of finger won’t straighten)
Causes
Most causes of phalanx fracture involve trauma to the fingers:
- Sudden “jamming” injuries to the fingers (mallet fractures)
- Twisting or hyperextension injuries (dog leashes, falls, sports)
- Blunt force trauma (work injuries, sports, vehicle accidents)
- Hand crush injuries
- Enchondroma (benign bone cyst that weakens the bone until it fractures)
Diagnosis
Fractures are obvious on physical examination, but severe sprains and contusions can also look and feel very much like a phalanx fracture. X-rays usually offer definitive diagnosis and help with treatment planning.
Why treatment matters
Suspected hand fractures warrant emergency treatment if you are experiencing hand numbness and tingling, severe or “tight” swelling, significant deformity of the hand or any open wounds around the hand (possible open or compound fracture). Even without these warning signs, it is best to seek urgent treatment.
Nonoperative treatment:
The results of delayed treatment of phalanx fractures can lead to undesirable outcomes such as nonunion (won’t heal) or malunion (heals crooked).
Splinting and buddy taping are the mainstays of nonoperative treatment for phalanx fractures. For many fractures, we start some early gentle motion, sometimes with hand therapy, to prevent permanent stiffness, but always follow the direction of your surgeon when it comes to moving or stretching a broken finger.

Operative treatment:
Surgical repair of phalanx fractures is required when the fracture pieces are unstable (won’t stay in place), or not healing properly with splint treatment. We give a mild sedation and a local block to numb the finger in the operating room. If the phalanx can be set straight, we place metal wires through the skin and into the bone to keep it straight while it is healing.
If the fracture is severe, we may need to make a small incision over the finger to restore the alignment of the broken phalanx directly and hold the pieces in place with tiny metal plate and/or screws. Often, a second surgery is performed after the bone has healed to remove the plate and screws if they are uncomfortable under the skin or cause finger stiffness.
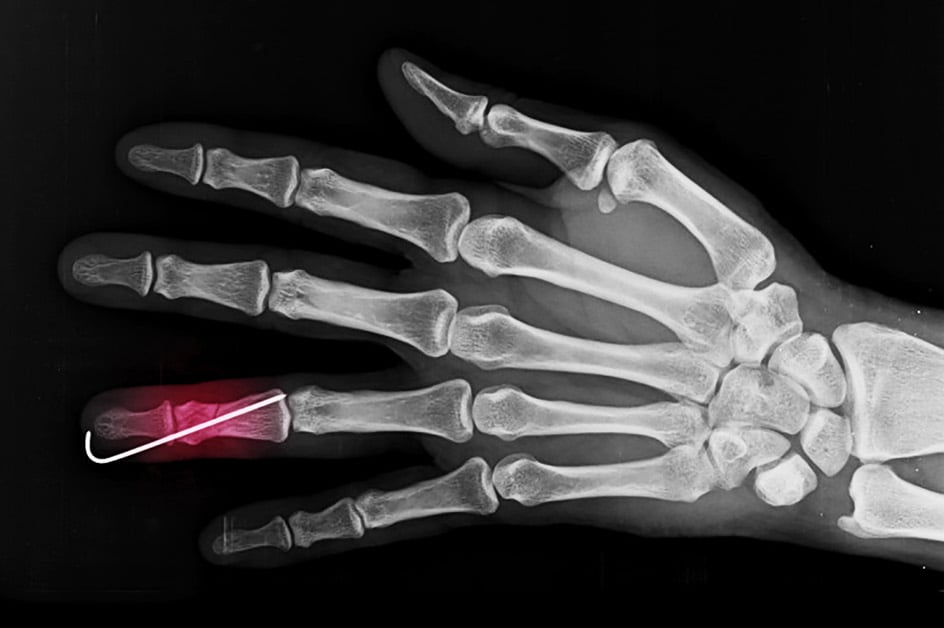 X-ray showing pinning in a finger to repair a Phalanx Fracture
X-ray showing pinning in a finger to repair a Phalanx Fracture
Overview
Take the next step
Our board-certified specialists are here to help you heal. They can often diagnose the problem in one visit and get you started with a personalized treatment plan. We offer a wide variety of treatment options.